mHealth Research
Recently my most active area of research interest is in mobile health applications, or mHealth apps. This interest grew out of collaborations at Children' National Health System in Washington D.C., and aligns with my orientation towards use-inspired research with social impact. As I've worked with multiple clinicians on fascinating clinical problems (mostly in pediatric chronic disease), I've noticed a dearth of technical insight in mHealth apps designed for behavioral change. This is not to say there is a lack of innovation; but I find many publications simply turn the wheel on incremental technology advancements, applying "technology feature X in digital health intervention (DHI) Y for patient population Z". I believe we must move past feature-of-the-moment (SMS, smartphone notifications, game platforms, social media instance) and look toward the future of how technology surrounds us and can deliver comprehensive health-related behavior change.
To this end my recent work focuses on multiple aspects of DHIs: 1) detailed interaction mining to dynamically construct and adapt just-in-time personalized delivery models that promote adherence with quality, 2) microintervention deliveries over time to achieve aggregate outcomes and sustained behavior change, and 3) applying computational thinking to DHIs, presently in the form of a proposed reference model and meta-language for interaction modeling (see NSF SCH poster and handout).
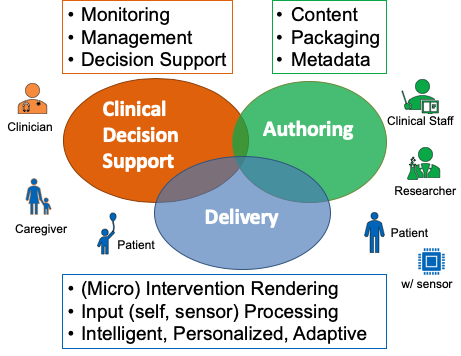
mHealth Projects (click image to expand)
-

COMPASS for Courage (formerly REACH for Success) is a preventative anxiety approach for middle-school kids. Developed by Ryan Stoll PhD, under the guidance of Armando Pina, PhD, COMPASS addresses anxiety disorders before they negatively impact school and quality of life outcomes. The REACH+ and COMPASS mHealth apps promote adherence to CBT skill practice in an age-appropriate design. In the context of this work we have piloted dynamic programming algorithms and adaptive personalized AI algorithms to achieve adherence outcomes.
-

BRIDGES is a family-focused program for middle school students and their parents. It uses evidence-based strategies to increase school engagement and keep teens on a positive path in life to prevent common teen problems. Long term follow-up shows Bridges increases high school graduation rates and reduces drug and alcohol problems in high school.
Currently we are designing DHIs around the skills development within Bridges to promote effectiveness at scale. We anticipate piloting our first mHealth app in Spring 2020.
Nancy Gonzalez is the inventor and primary collaborator on Bridges. You may find out more here.
-
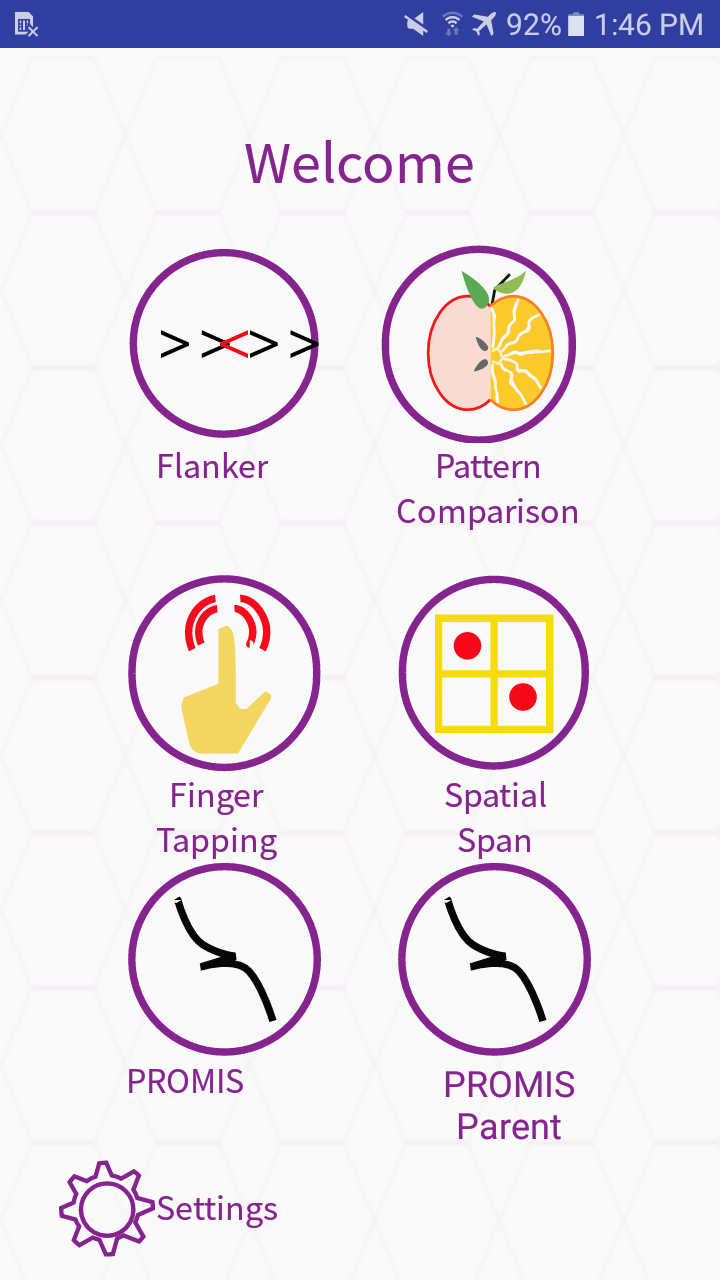
BrainTracker is an mHealth app and clinical decision support portal for remote assessment of quality of life comorbidities of pediatric epilepsy. BT supports 4 validated interactive neuro-physiological tests with self-reporting (subject and care giver) providing more frequent qualoty assessment of remote patients who cannot come in to a clinic frequently.
The mHealth platform is designed and implemented using flexible and adaptive APIs supporting a range of dynamic configurations for assessment.
Madison Berl, PhD of Children's National Health System is the primary collaborator on BrainTracker.
-

Aspira is a home asthma monitoring platform for monitoring children with asthma. The system integrates physical devices (an indoor air quality monitor and a digital spirometer), a serious game on a tablet, data gathering processes on the tablet, and data management and reporting capabilities on a server. The result is a system which encourages children to take proper spirometer readings, and a low-cost platform for adapting behaviors to indoor air quality.
The 1st generation Aspira was built in collaboration with Children's National Health System (CNHS), Kevin Cleary PhD and Dr. Ivor Horn MD as collaborators.
Second-generation Aspira was developed under an R41 NIH grant (STTR) in collaboration with CNHS, Seattle Children's Hospital, ASU, and Mad*Pow of Boston (PI).
-
This mobile application implements a survey for collecting pain scores and pain burden reporting for patients with Sickle Cell Disease (SCD). The goal of this application is to assist with pain management and eventually result in reduced hospital readmissions for patients with SCD. In our technical research we used gamification techniques and detailed interaction mining to encourage pain reporting with quality
The PI of this project is Dr. Zenaide Quezado, National Institutes of Health (NIH)) in conjunction with Kevin Cleary, PhD, Sheik Zayed Institute at CNHS.
Selected Publications
- Gary, K., Rallabhandi, P., Quezado, Z., and Cleary, K. “A Pain Reporting Platform for Adolescents with Sickle-Cell Disease”. The 52nd Hawaii International Conference on System Sciences (HICSS-52), January 2019.
- Stoll, R.D., Pina, A.A., Gary, K. & Amresh, A. (2017). Usability of a Smartphone Application to Support the Prevention and Early Intervention of Anxiety in Youth. Cognitive and Behavioral Practice. doi:10.1016/j.cbpra.2016.11.002
- Gary, K., Stoll, R., Rallabhandi, P., Patwardhan, M.*, Hamel, D., Amresh, A., Pina, A., Cleary, K. and Quezado, Z. (2017). “MHealth Games as Rewards: Incentive or Distraction?” Proceedings of the ACM International Conference on Digital Health, London UK, July 2017.
- Patwardhan, M, Stoll, R., Hamel, D.B., Amresh, A., Gary, K.A. and Pina, A., “Design a Mobile Application to Support the Indicated Prevention and Early Intervention of Childhood Anxiety”, Proceedings of the National Institutes of Health Conference on Wireless Health (WH’15), Bethesda, MD, October 2015.
- Amresh, A., Lyles, A., and Gary, K. "Game Based Behavior Change Methods in Healthcare: The Case of Obesity", in Cognitive Informatics in Health and Biomedicine Understanding and Modeling Health Behaviors, (Patel, V.L., Arocha, J.F., & Ancker, J.S. eds.) Springer, 2017
- Heath, C., Baron, T., Gary, K. and Amresh, A. "Reflection on Assumptions from Designing Female-Centric Educational Games", Proceedings of the 2nd International Conference on Serious Games, Brisbane, Australia, September 2016.
Funding
- "Software Support for an mHealth Application monitoring Sickle Cell Disease", contract to Children's National Health System, $6,000, 2014
- "Mobile Application Development Support", Joseph E. Robert Jr. Foundation. Total Award $30K (PI, Dr. Zenaide Quezado, CNHS). ASU share $18K. Period of Performance August 2014 - August 2015.
- "Software Support for a Home Asthma Monitoring Platform", contract to Children's National Health System, $9,600, 2013-14
- "Improving Asthma Control through mHealth-Based Home Monitoring", NIH STTR Phase I, RFA-MD-13-009. Total Award $225K (Mad*Pow PI, Dr. Ivor Horn, Seattle Children's Hospital clinical PI). August 2014 - August 2016.
- Quezado, Z., Cleary, K., and Gary, K. “SCD-PROMIS: A software platform for enhanced self-efficacy and patient-provider engagement for children with sickle cell pain” $500K. Pfizer Foundation, 2015-17.